Every penny donated to us matters. So, we want you to know how that money is being spent for the benefit of children with cancer. With that in mind, each month we share an update from one of our research teams so you can see the progress being made. All because of your support.
We recently caught up with the Advanced Radiotherapy team at The University of Manchester. Over the coming year, they are working on a project, funded by Friends of Rosie, looking at ways to reduce the risk of facial asymmetry following radiotherapy for childhood cancer. Here, researcher Abigail Bryce-Atkinson shares their first project update.
Project Update

Explains Abby, “Radiotherapy is a key part of treatment for many children diagnosed with cancer. However, it can result in short and long term side effects that can affect the quality of a child’s life in the future. For example, up to 75% of children treated for head and neck rhabdomyosarcoma (a type of soft tissue cancer) will experience some degree of facial underdevelopment.
“Over the next year, thanks to the funding from Friends of Rosie, we aim to develop methods that will help us determine the relationship between the dose of radiotherapy and regions of the face that may be important in preventing facial asymmetry in children treated for cancer.”
Using imaging data to reduce side effects
Continues Abby, “The core focus of our research group is using computer programmes and simulations to analyse radiotherapy and imaging data from many patients treated. This will help us to inform future practice and improve how radiotherapy is delivered, so that it has fewer side effects.
“Our group has developed a method called “image-based data mining”, or IBDM, which allows us to efficiently process large amounts of radiotherapy data. In this method, we use the data from pre-treatment imaging and the radiotherapy dose distributions to identify specific regions of the anatomy that are sensitive to radiation.
“To do this, we perform a process called image registration. This is matching or deforming one image to another to register all images from different patients to one reference image. We also do this for the dose distributions. Then we correlate the information from each position (or voxel) in the image with an outcome, such as facial asymmetry, to identify linked regions. Take a look at the diagram below to see how it works.”
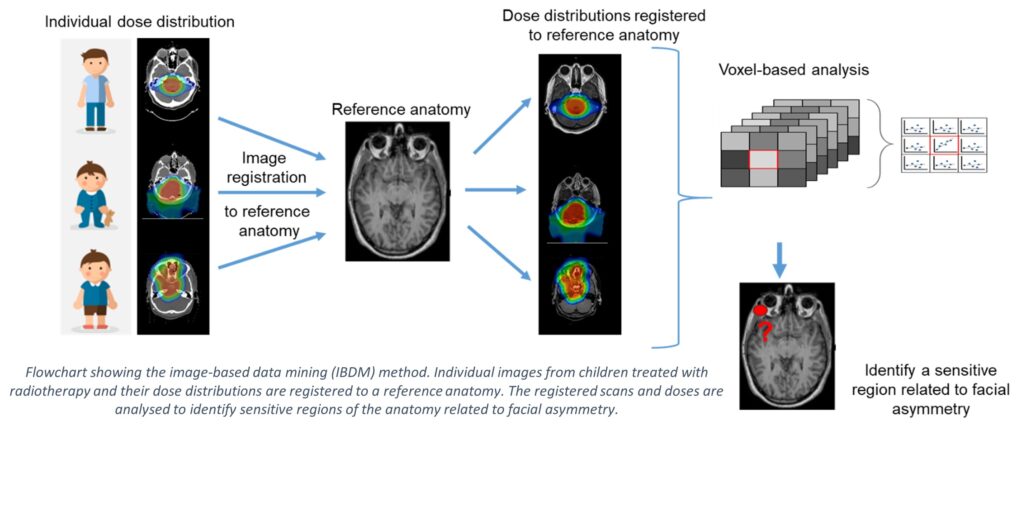
We have seen the effectiveness of this method in data from adults treated for lung, head and neck cancers. For example, researchers identified a specific muscle in the jaw as a sensitive region affecting the ability to open the mouth fully after radiotherapy of the head and neck.
Adults vs. Children
Continues Abby, “To apply this method to data from children, we need to account for the differences in their anatomy compared to adults. Since children are still growing, there will be differences in growth and development between children of different ages, such as head size and dental development. The first steps of this project are to measure these differences and see how they affect the performance of the IBDM method outlined above.
“Ultimately, we hope to use this method to help enable “smarter” treatments by identifying regions that could be spared radiotherapy dose to help decrease the risk of facial asymmetry in the future.
“Our thanks go to Friends of Rosie and all your supporters for funding this vital research. We look forward to updating you with our progress throughout 2021!”
What this means in reality – Emma’s experience
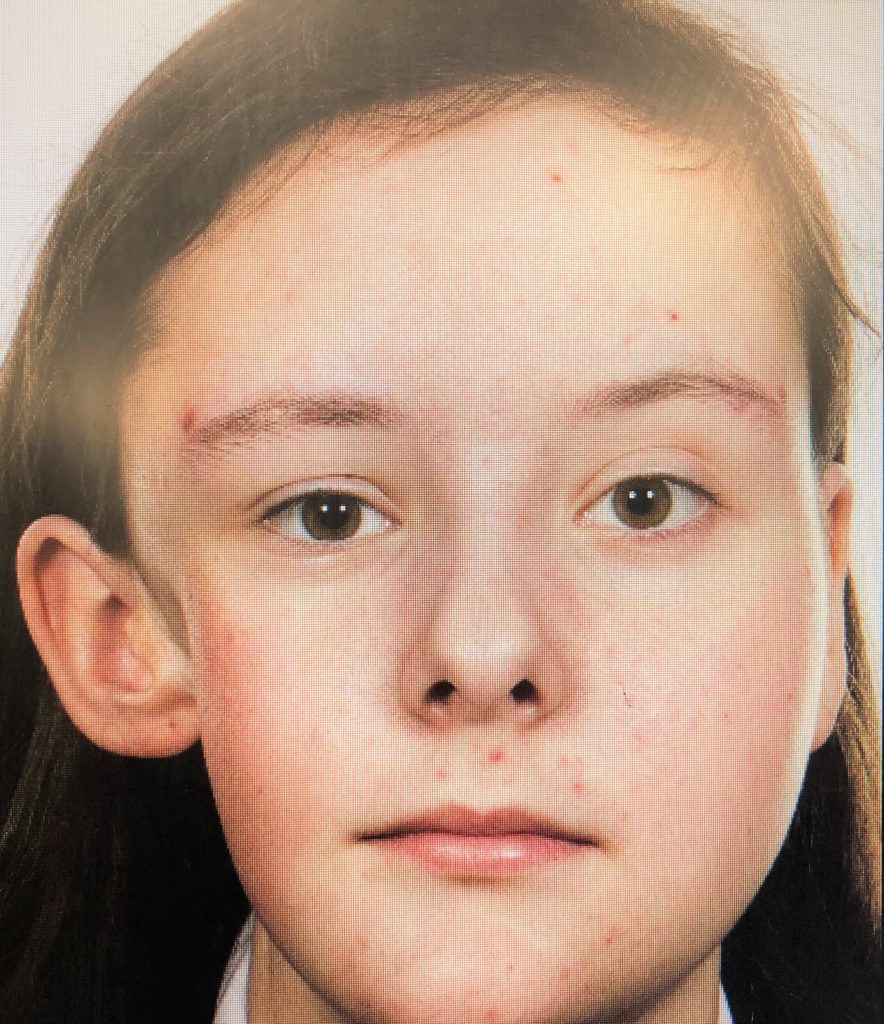
One family who are closely following this project are the Paytons. Emma Payton was eight when she was diagnosed with Alveolar Rhabdomyosarcoma. It was wrapped around her cheekbone and was in her masseter muscle. She received nine rounds of chemotherapy, had an operation to remove remaining tumour, and had 23 doses of radiotherapy.
Emma’s mum, Tracey, explains, “For us, receiving NHS funded Proton Beam Therapy in Oklahoma was such a fantastic opportunity. We knew this would minimise the risk to Emma’s development, but we also knew the side effects were (and still are) relatively unknown. We were warned of potential disfigurement. But, we also knew we had no choice but to have the treatment to improve Emma’s chances of a full recovery. We’d deal with the rest when we needed to.
“For a while, her disfigurement wasn’t too noticeable. However, as she began to develop and reach puberty, it became very pronounced and Emma also became more aware of her looks. She had always maintained that she didn’t care about it. But, as the pressures of being a teenager kicked in, she decided she would like reconstruction on that side of her face.
“Unfortunately, this was all being dealt with as Covid hit, so it’s unlikely the surgery will happen any time soon. As grateful as we are, this feels like another hurdle she needs to face despite her cancer treatment ending seven years ago.
“If there were a way to treat children and avoid this upheaval further down the line, then this would be such a huge relief to families who have already been through so much. We’re delighted that this research is taking place and our thanks go to everyone involved in this project. A special thanks also to Friends of Rosie and your supporters for continuing to champion research for children’s cancers.”




